Why the New Wound Closure Device Is a Must-Have for Modern Surgeons
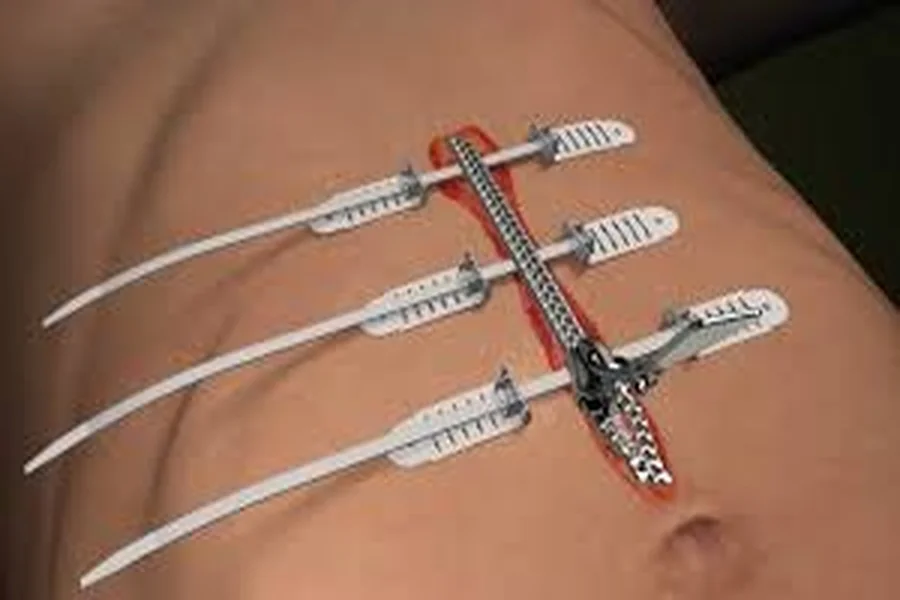
In the ever-evolving field of surgery, the introduction of new technologies often challenges established practices. One such innovation, the New Wound Closure Device, has raised questions about whether traditional methods of wound closure, such as suturing and stapling, are still the best options. In this article, we explore why the new wound closure device is rapidly becoming an essential tool for modern surgeons, and why it may soon replace older methods for good.
Challenging Traditional Wound Closure Methods
While traditional methods like sutures and staples have served surgeons well for decades, they are not without their limitations. Suturing, for example, can be time-consuming and requires significant skill and precision to avoid complications like tissue damage, uneven closures, and increased risk of infection. Similarly, staples may leave behind visible scars and sometimes cause discomfort or irritation.
The New Wound Closure Device offers an alternative that addresses these issues head-on. By utilizing advanced technology, this device streamlines the wound closure process, providing surgeons with a faster, more reliable, and more efficient way to close wounds without sacrificing quality. The device’s ability to create a secure, consistent closure in a fraction of the time makes it an invaluable tool for busy surgical teams.
As healthcare professionals continue to seek ways to improve outcomes and optimize surgical workflows, the new wound closure device is emerging as a game-changer that challenges the status quo and sets new standards in the industry.
Speed and Efficiency: A Game-Changer for Surgeons
One of the main benefits of the New Wound Closure Device is the speed at which it enables surgeons to close wounds. Traditional sutures can take significant time to apply, especially in large or complex incisions. The new device, on the other hand, offers rapid closure without compromising the quality of the wound seal. This reduction in procedure time is especially valuable in high-stakes surgical environments, where every minute counts.
Not only does this increase surgical throughput by allowing more procedures to be completed within the same timeframe, but it also reduces the time patients spend under anesthesia. This can significantly lower the risks associated with prolonged sedation, such as post-operative complications and delayed recovery times.
For surgical teams operating under time constraints or high patient volumes, the New Wound Closure Device represents a major improvement in operational efficiency, enabling surgeons to focus on other critical aspects of the procedure while achieving optimal results.
Enhanced Precision and Consistency
Another reason why the New Wound Closure Device is becoming indispensable is its ability to offer greater precision and consistency than traditional methods. While manual suturing is highly dependent on the surgeon’s skill, the new device delivers a consistent, even closure with every use. This reduces the potential for errors such as uneven suturing or gaps in the wound closure, both of which can lead to complications such as infection or delayed healing.
The precise nature of the new wound closure device also ensures that the wound edges are aligned correctly, promoting optimal healing and reducing scarring. For surgeons, this translates into more predictable and reliable outcomes, leading to improved patient satisfaction and faster recovery times.
Moreover, the consistent results provided by the new device allow surgeons to confidently perform procedures without worrying about variability in the closure process. This reliability is essential for maintaining the highest standards of care and ensuring that patients receive the best possible treatment.
Lower Risk of Infection and Complications
Infection is one of the most common complications following surgery, and traditional wound closure methods are not immune to contributing to this risk. The New Wound Closure Device helps to mitigate this risk by creating a tighter, more secure wound closure that prevents bacteria from entering the wound site. The secure closure reduces the likelihood of wound dehiscence (wound reopening) and other issues that can lead to infections.
Furthermore, the quick and efficient application of the device minimizes the time the wound is exposed to external contaminants. This not only reduces the risk of infection but also helps promote faster healing by minimizing unnecessary exposure to the environment during the closure process.
For healthcare facilities focused on improving patient outcomes and reducing the likelihood of post-operative complications, the new wound closure device is a key tool in enhancing the overall safety and success of surgical procedures.
Cost-Effectiveness and Long-Term Value
While the initial investment in a New Wound Closure Device may be higher than traditional suturing methods, the long-term value it provides makes it a worthwhile investment for many healthcare providers. The device’s speed, efficiency, and precision contribute to lower operational costs by reducing procedure times, improving patient recovery rates, and minimizing the risk of complications that can lead to additional treatments or longer hospital stays.
Moreover, the increased efficiency in the operating room allows hospitals to perform more surgeries with fewer resources, maximizing the use of operating rooms, staff, and equipment. This, in turn, helps healthcare providers achieve a better return on investment while ensuring high-quality care for patients.
The reduced risk of complications, combined with the time savings and improved outcomes, makes the new wound closure device an excellent investment for healthcare facilities looking to improve surgical efficiency without compromising patient care.
Conclusion
The New Wound Closure Device is quickly becoming an essential tool for modern surgeons. By offering faster, more precise wound closures, the device addresses many of the limitations of traditional methods, such as time consumption, variability, and risk of complications. Its ability to streamline surgical workflows, reduce infection rates, and promote faster recovery makes it an invaluable addition to any surgical team’s toolkit.
For healthcare providers seeking to enhance their surgical practices, the new wound closure device provides a combination of efficiency, precision, and safety that can significantly improve patient outcomes and operational efficiency. For more information on how this innovative tool can benefit your surgical team, visit this comprehensive guide
